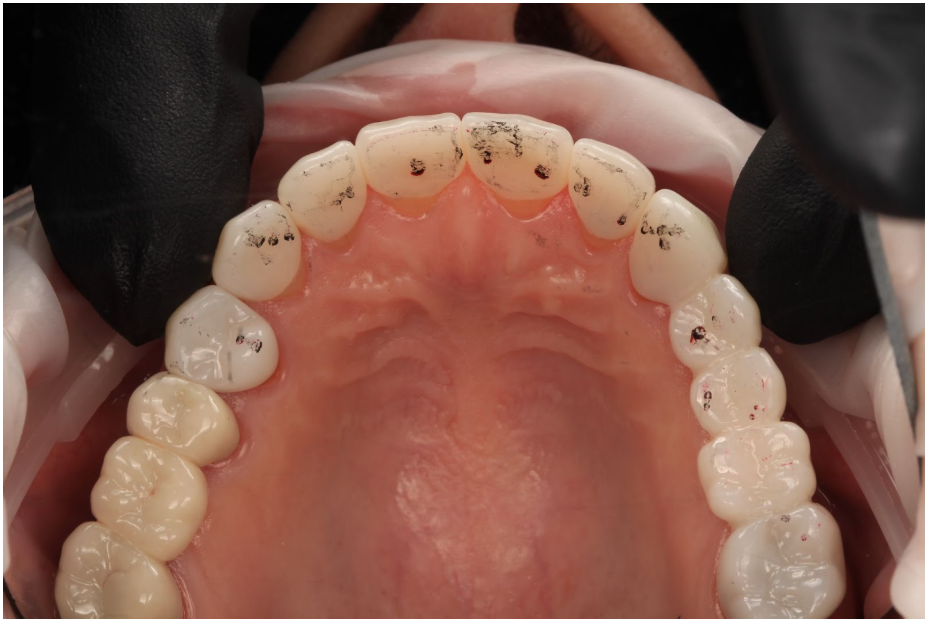
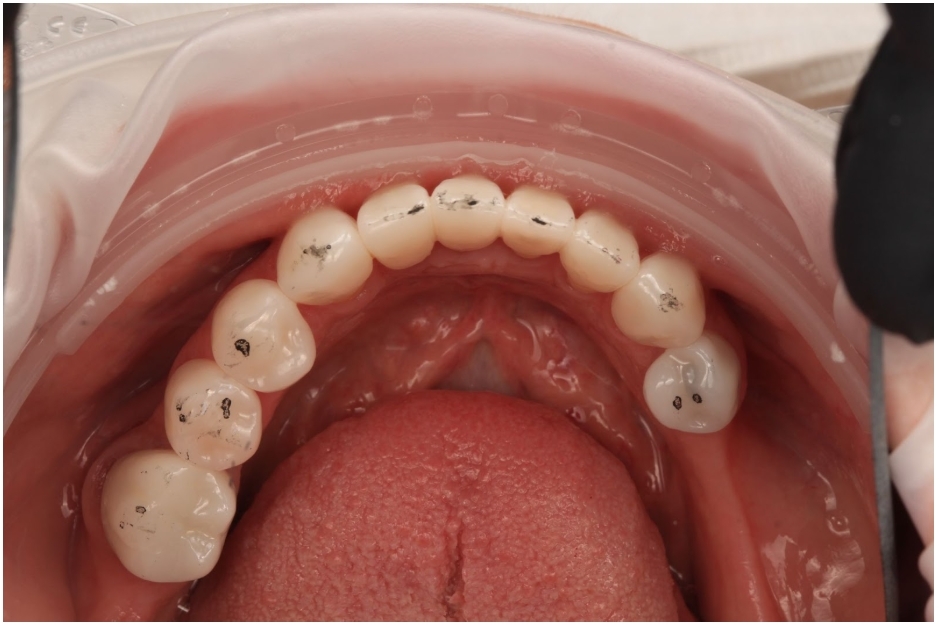
Articulating paper is the most universally used tool in clinical dentistry. Every dental school teaches it. Every clinic stocks it. The workflow is ingrained: have the patient tap, examine the marks, and adjust whatever looks heavy.
But what does the evidence actually say about articulating paper? Is it accurate? Is it reliable? And can clinicians interpret the marks it produces?
The short answer to all three is no. And understanding why should change the way every dentist checks and adjusts occlusion.
The most fundamental issue with articulating paper is one that’s easy to overlook: it has physical thickness. Depending on the product, that can range from as thin as 8 microns to over 200 microns. When we place it in the mouth, we’re no longer recording the native tooth-to-tooth occlusion. We’re recording a modified occlusion — one that only exists because the paper is there.
This isn’t theoretical. Helms, Katona & Eckert (2012) tested six different occlusal indicator products and measured the three-dimensional forces and moments on occluding teeth with and without the indicators in place. All six products — including thin articulating papers — produced statistically significant differences in forces and moments compared to direct tooth-to-tooth contact (P < 0.05).
Mitchem, Katona & Moser (2017) extended this to full dentitions using a dentiform in Class I centric occlusion. The conclusion was stark: popular occlusal detection products alter the occlusal contact forces, and therefore their markings cannot characterize the actual occlusion.
So the paper changes the very thing it’s supposed to measure.
The problems go further. Saad et al. (2008) compared thick (60 μm) and thin (25 μm) articulating papers at loads of 100N, 150N, and 200N. The thicker paper produced significantly more marks and larger marks than the thinner paper (p ≤ 0.02–0.0001). But here’s the critical finding: there was no significant increase in the number or size of marks with increased load for either material. The paper thickness influenced the markings more than the actual force applied. This means the paper is generating false positive contacts that don’t exist at the tooth-to-tooth level.
And the markings aren’t even reproducible. Gazit, Fitzig & Lieberman (1986) compared consecutive occlusal records and records taken at one-month intervals. Neither articulating paper nor photoelastic wafer techniques were found to be highly reproducible.
So even when used purely as a contact locator, articulating paper provides an approximation contaminated by false positives and, in many cases, false negatives.
The traditional teaching — passed down through occlusion textbooks for decades — is that larger, darker articulating paper marks indicate heavier occlusal force, and smaller, lighter marks indicate lighter force. This forms the basis for how most clinicians decide which contacts to adjust.
There is no scientific evidence supporting this.
Carey et al. (2007) applied controlled, incremental compressive loads from 25N to 450N on epoxy dental casts with articulating paper interposed. Six hundred markings were photographed and analyzed. No direct relationship between paper mark area and applied occlusal load could be found. While there was a general trend of increasing mark area with increasing load, the variability was enormous — different teeth at the same load produced significantly different mark sizes approximately 80% of the time. The authors concluded that operators should not assume the size of paper markings accurately describes the occlusal contact force content.
Qadeer et al. (2012) moved from bench testing to in vivo. Thirty subjects had their occlusal contacts marked with articulating paper strips, followed by computerized occlusal analysis force recordings. The largest, darkest paper mark in each quadrant matched the most forceful tooth in that quadrant only 38.3% of the time. The coefficient of determination was r² = 0.067 — meaning only approximately 7% of the paper mark’s surface area could be explained by applied occlusal force. The remaining 93% was attributable to factors unrelated to applied occlusal force.
To put it plainly: the marks are overwhelmingly shaped by tooth anatomy and contact area geometry, not by how much force is at that contact. When we look at a big dark mark and decide it’s a “high spot,” we’re reading the wrong variable.
Given that mark size doesn’t correlate with force, it shouldn’t be surprising that clinicians can’t reliably interpret paper marks. But the degree of failure is striking.
Kerstein & Radke (2014) presented six occlusal-view photographs of articulating paper marks to 295 dentists. Each clinician was asked to identify the most and least forceful contacts — later compared against computerized occlusal analysis measurements. The mean correct score was 1.53 out of 12 possible answers. 94% of participants scored 3 or fewer. Years in clinical practice made no significant difference (P > 0.16). Number of occlusion CE courses taken made no difference (P > 0.75). Experience did not improve accuracy.
Sutter (2018) replicated this with a digital poll of 152 dentists. The mean correct response was 13.13%. Random chance was calculated at 16.7%. The dentists performed worse than guessing.
Basson, Kerstein & Radke (2020) conducted another replication. Out of 246 total contact choices made by the participants, only 12 were correct — a 4.88% accuracy rate.
Shetty & Chowdhary (2023) tested prosthodontists specifically, using both 40-micron and 100-micron articulating paper. Only four participants chose any correct answers with the 100-micron paper. With 40-micron paper, there were zero correct answers.
This isn’t a knowledge problem or a training problem. It’s a fundamental limitation of subjective visual interpretation applied to a tool that was never designed to convey force information.
So what do we have? A material that doesn’t accurately record the native occlusion. That generates false positive contacts from its own thickness. That produces marks whose size is unrelated to force. And that clinicians — including specialists — cannot reliably interpret.
And we’re making irreversible adjustments to teeth and restorations based on this.
I still use articulating paper every day. It has a role. But I never adjust based on only the markings I see. I have to confirm those markings — and that is done with shimstock.
Shimstock (typically 8–12 μm metallic foil) provides something articulating paper cannot: a binary, reliable answer. Is there a true contact, or isn’t there? Hold or no hold. No subjective interpretation. No guessing. No false positives from material thickness — or at least not within 10 microns.
Articulating paper can supplement shimstock by providing a visual map of approximate contact location. But shimstock is what confirms whether a contact is real. That’s what I need verified before I pick up a handpiece.
Before adjusting any occlusion. Don’t adjust based on what a paper mark looks like. Verify with shimstock which contacts are real first, then use the paper marks as a map to locate them.
Before and after any localized restorative work. Before you prep, verify and document contacts with both articulating paper and shimstock so you have a baseline. After you seat the restoration, reconfirm those same contacts with shimstock. That’s how you know you’ve accurately restored the occlusion — particularly for straightforward restorative work where the goal is not to change the vertical dimension or occlusal relationship.
Articulating paper is an approximation. Shimstock is a verification. I recommend using both — but don’t trust the articulating paper.
1. Carey JP, Craig M, Kerstein RB, Radke J. Determining a relationship between applied occlusal load and articulating paper mark area. Open Dent J. 2007;1:1–7.
2. Saad MN, Weiner G, Ehrenberg D, Weiner S. Effects of load and indicator type upon occlusal contact markings. J Biomed Mater Res B Appl Biomater. 2008;85(1):18–22.
3. Qadeer S, Kerstein R, Kim RJY, Huh JB, Shin SW. Relationship between articulation paper mark size and percentage of force measured with computerized occlusal analysis. J Adv Prosthodont. 2012;4(1):7–12.
4. Kerstein RB, Radke J. Clinician accuracy when subjectively interpreting articulating paper markings. Cranio. 2014;32(1):13–23.
5. Sutter BA. A digital poll of dentists testing the accuracy of paper mark subjective interpretation. Cranio. 2018;36(6):396–403.
6. Basson E, Kerstein RB, Radke J. Ability to correctly select high force occlusal contacts from articulating paper markings. Adv Dent Tech. 2020;2(1):101–110.
7. Shetty PP, Chowdhary R. Prosthodontists’ clinical accuracy in selecting high force occlusal contacts from articulating paper marks — A questionnaire study. Adv Dent Tech. 2023:1–15.
8. Helms RB, Katona TR, Eckert GJ. Do occlusal contact detection products alter the occlusion? J Oral Rehabil. 2012;39(5):357–363.
9. Mitchem JA, Katona TR, Moser EAS. Does the presence of an occlusal indicator product affect the contact forces between full dentitions? J Oral Rehabil. 2017;44(10):791–799.
10. Gazit E, Fitzig S, Lieberman MA. Reproducibility of occlusal marking techniques. J Prosthet Dent. 1986;55(4):505–509.